Polymyalgia Rheumatica Print Page
Overview
Polymyalgia rheumatica, or PMR, can cause significant pain and stiffness, primarily focussed around the shoulder and hip muscles. It can be disabling. Fortunately, treatment is available and works quickly and effectively for most people.
What is Polymyalgia Rheumatica?
- Polymyalgia Rheumatica, or PMR, is an autoimmune disease which can cause significant pain and stiffness in the muscles around the shoulders and hips.
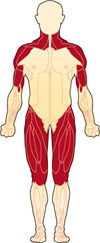
PMR: Proximal muscle
involvement (noted in red)
Why does Polymyalgia Rheumatica happen?
- No one really knows. There is as of yet an unidentified trigger which causes your immune system not to recognize certain cells in your body as belonging to you. Because of this, they attack them, causing the clinical symptoms.
Is there something I could have done to prevent PMR?
- Because we do not fully understand why PMR happens, we do not know if anything could prevent it. There may be a genetic predisposition, but it has not been clearly identified yet.
Who gets PMR?
- The greatest risk factor for PMR is age, with virtually all patients over the age of 50, most older than 60.
- Women are twice as likely to develop PMR than men.
What are the symptoms in PMR?
- Most patients with PMR describe pain and stiffness worse in the areas around the shoulders and hips muscles, equal on both sides. Some patients describe weakness, although it is pain which is limiting strength. The pain often limits mobility and day to day activities. The stiffness can be profound, usually worse in the morning.
I have some of the symptoms listed above. Does this mean I have PMR?
- While it is possible, there are many other conditions which need to be considered.
How is Polymyalgia Rheumatica diagnosed?
- PMR can usually be diagnosed by a rheumatologist after he/she performs an appropriate history and physical examination with you. Your physician will also do a blood test checking for markers of inflammation in the blood. While these are not specific for PMR, they are usually elevated in patients who have this diagnosis.
Are there any other conditions associated with PMR?
- There are two other diseases which can occur around the time of having PMR.
- Giant Cell Arteritis, a type of vasculitis, which can cause new headaches, scalp tenderness and potentially sudden blindness, is associated with PMR in a minority of cases.
- Rheumatoid Arthritis can occur at the same as PMR, or even sometimes a few months after PMR is diagnosed.
I have been diagnosed with PMR. How is it treated?
- PMR is treated with a low dose steroid, prednisone, usually between 10 and 20mg per day. If the diagnosis is correct, most patients will feel at least 90% within a week if not a few days.
- Most rheumatologists will slowly lower the dose prednisone over 6-12 months until it is stopped. By decreasing the dose slowly, it prevents recurrence of symptoms and allows patients to remain in remission off medications.
- Because patients will be on prednisone for more than 3 months, there is an increased risk of developing osteoporosis. Patients should be instructed to take supplemental Calcium and Vitamin D daily. Most patients are also prescribed a bisphosphonate, a class of medication which reduces the risk of thinning bones.