Osteoporosis Print Page
Overview
Osteoporosis occurs when there is a reduction in the mass in one’s bones. So called “thinning of the bones” increases your chance for bone fracture, particularly the back, hip or wrist. There are many risk factors for developing osteoporosis, some of which can be prevented. For those with osteoporosis, there are treatment options available which can reduce your chance for fracture.
Frequently Asked Questions
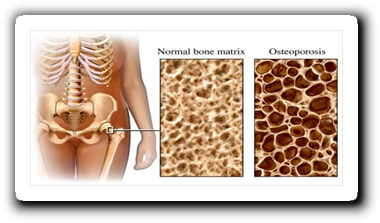
What is osteoporosis?
- Bone consists of two key components called hydroxyapatite and osteoid. In osteoporosis, there is a reduction of both of these components of bone.
Are osteoporosis and osteoarthritis the same thing?
- While they sound similar, they are in fact very different conditions. Osteoarthritis is a problem with joints which can cause pain and functional disability. Osteoporosis is bone thinning. Unless you break a bone, it does not directly cause pain or disability. Click here for more information on osteoarthritis.
Why does osteoporosis happen?
- Bone formation is regulated by two cell types, one causes bone formation (osteoblasts) and one causes bone breakdown (osteoclasts). In normal healthy bone, these cells work together, slowly breaking down older bone and replacing it with new bone over long periods of time. In osteoporosis, bone breakdown occurs faster than bone formation, reducing the overall bone mass.
Why is having thinner bones a problem?
- Patients with osteoporosis have an increased risk for breaking their bones. Further, these fractures can happen with minimal trauma. The most common fractures seen in osteoporosis are fractures of the hip, vertebrae and wrist.
How common is osteoporosis?
- Osteoporosis is very common. Some studies estimate 50% of people over the age of 55 may have osteoporosis and many more at risk for developing osteoporosis. The majority are women.
What are risk factors for developing osteoporosis?
- There are many factors which may increase your risk for developing osteoporosis. Some of these cannot be prevented. They include:
- Increasing age
- Female gender
- Early Menopause
- A family history of an osteoporotic fracture
- A previous fracture thought to be due to osteoporosis
- Certain diseases, including but not limited to rheumatoid arthritis, hyperparathyroidism, and hyperthyroidism
- Many other risk factors can be reduced, including:
- Smoking
- Excessive Alcohol Use
- Excessive Caffeine Intake
- Low Weight
- Poor Calcium Intake
- Certain medications, including glucocorticoids (steroids).
How do I know if I have osteoporosis? Does it hurt?
- Most people who have osteoporosis do not know it unless they get tested.
- Unless you have had a fracture, it should not cause pain.
- Some people with osteoporosis may notice loss of weight, or more of a stoop in their back, which can be due to undiagnosed verterbral fractures.
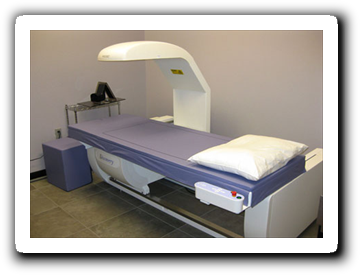
What is the test for osteoporosis?
- Osteoporosis is best tested for using a machine called a DEXA scan. It is a very low radiation safe test which measures the bone density of the lower back and hip.
If I am diagnosed with osteoporosis, what is my risk of breaking a bone?
- The risk of fracture depends on many different things. While your bone density as measured by the DEXA scan is an important component to determine your risk, it is also important to consider your age, previous fractures, other medical conditions and medications. It is important your doctor has all this information to help determine your risk.
- With the appropriate information, you and your physician can estimate your risk of breaking a bone over the next 10 years as either low (<10%), medium (10-20%) or high (>20%).
My doctor told me I have osteopenia. Is that the same as osteoporosis? Does this need treatment?
- Osteopenia is a term that has been used for patients who demonstrate low bone mass on DEXA scan, but not low enough to be called osteoporosis.
- Treatment may or may not be recommended, depending on your age and other risk factors you may have for a fracture.
I have been told I should consider treatment for osteoporosis.
- There are many medication options available for osteoporosis, with a class of medications called bisphosphonates being the most common. Discuss with your physician which is right for you.
- There are also some very important steps which you can take which are not prescribed by your physician. They include:
- Dietary changes (click here for some ideas)
- Daily calcium intake: 500mg three times per day
- Daily Vitamin D intake: 800-2000 Units per day
- Regular weight bearing exercise (E.g. walking)
I do not have osteoporosis, but I have been started on glucocorticoids (steroids/prednisone).
- Glucocorticoids can cause a significant loss of bone mass, particularly for those using them for at least 3-6 months. Patients who require glucocorticoids for at least this long should discuss with their physicians whether or not preventative treatment for developing osteoporosis is right for them.
What can I do to reduce my chance of developing osteoporosis?
- There are many things we can all do to improve our bone health, starting as children and throughout our lives. They include:
- Daily calcium intake. Children should have at least 800mg of calcium daily either through diet or supplement, while adults over the age of 50 should have 1500mg per day.
- Daily Vitamin D intake between 800-2000 units daily.
- Regular weight bearing exercise.
- For some tips on foods that may help, click here.
What else is important to know about osteoporosis?
- Remember: The ultimate goal of treating osteoporosis is not necessarily making the bones strong again. The goal is to safely lower your risk of breaking a bone.